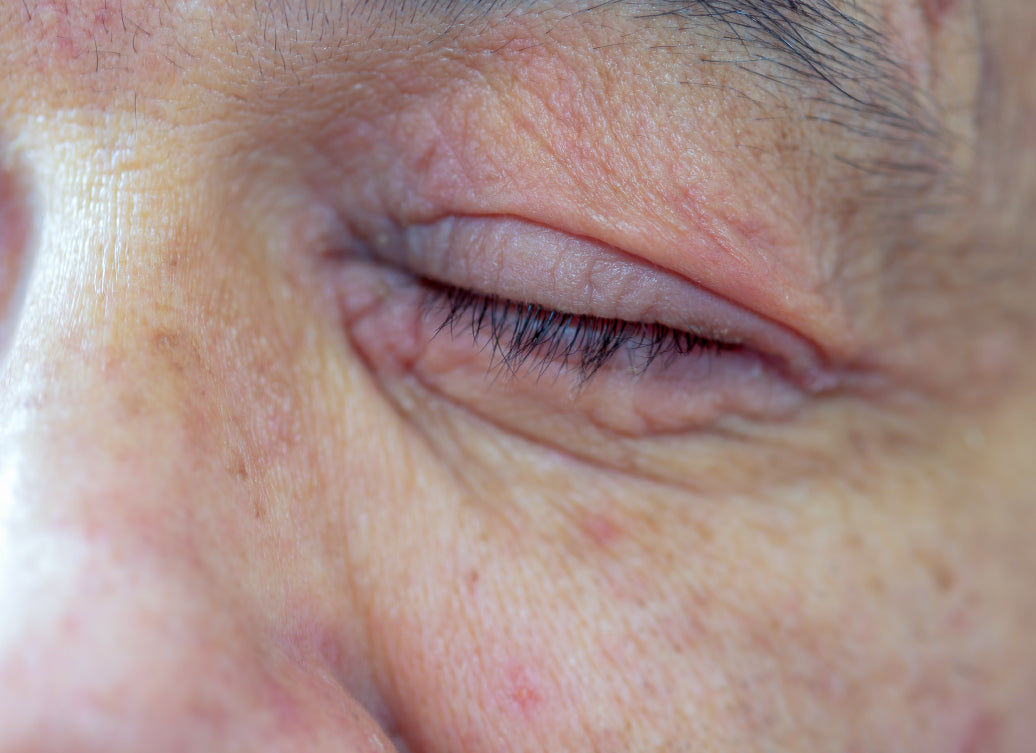
Periocular dermatitis is diagnosed when the skin around the eye is inflamed and irritated, but behaves in a particular way. Like its close (literally) relative, perioral dermatitis, the periocular variety can appear as a rash, as spots, pustules or dry and itchy skin.
Periocular dermatitis isn’t just dermatitis that happens to occur around the eyes, though; it’s a bit more complicated than that, because it has specific characteristics which make it different to temporary skin irritation.
It’s a persistent condition, one that seems to get better but then recurs without any clear reason; periocular dermatitis can disappear for weeks, months or even years, then flare up again in reaction to something. In this regard, periocular dermatitis is similar to perioral dermatitis or papulopustular rosacea, which are also persistent and tricky to manage. In fact, it’s classed as a variant of the rosacea family, another condition that occurs in waves of flare-ups, seems to affect one demographic more than another (pale skinned women aged 20-50), and is often associated with sun exposure.
There’s evidence that a flare of periocular dermatitis is made worse by various things, but every sufferer will have slightly different triggers, and what flares one person up might be perfectly well tolerated by another. Getting to the bottom of what affects you and your skin is key to being able to manage the condition!
So what sort of things could be making a periocular flare worse? Here are a few possible candidates:
Diet: some doctors have suggested a link between perioral and peculiar dermatitis and diet, with gluten and sugar being a particular concern.
An impaired skin barrier function: as with eczema sufferers, impaired barrier function has a genetic component, as well as an environmental one. Although there’s nothing you can do about an inherited problem, there are ways to support your skin barrier, with oily emollients and with regenerative nutrients.
Microflora: if your skin’s microflora is out of balance, then flares are either made more likely or worsened. These are microorganisms which live on the skin, and can be bacteria, fungi or mites; too many and the skin can erupt.
Topical steroids: for some people, the treatment can become the cause. Topical corticosteroids have been shown to be responsible for outbreaks of periorificial (i.e. both perioral and periocular) dermatitis, as well as papulopustular rosacea.
Cosmetics & skincare: irritant ingredients in things you put on your face such as makeup, face washes, thick face creams, sunscreens, and cosmetic skincare treatments have all been shown to exacerbate periorificial dermatitis, and are best avoided, especially during a flare.
Hormones: oral contraceptives, hormonal changes and hormonal supplements have all been implicated in periocular dermatitis, but more research is needed.
Stress: like so many skin conditions, periocular dermatitis is worsened by stress, because of the way the body reacts to stress or anxiety with inflammatory response, which in turn affects the skin.
Environmental conditions: bright sunlight, strong winds, UV light, extremes of temperatures can all aggravate a flare.
What can you do about it? Well, the most obvious thing is to avoid whichever culprit might be causing the problem - though that is easier said than done! Most doctors would advise as a first crucial step that you stop putting anything on your face until the flare is over, except for the absolute mildest of unscented emollients.
For more ideas about how to manage the condition, see our article How To Treat Perioral Dermatitis, which covers a lot of the same ground.
Recommended products for skin prone to periocular dermatitis:
Balmonds Skin Salvation
with hemp and beeswax
Balmonds Omega-Rich Cleansing Oil
with rosehip and calendula